What Should Men in Minneapolis Know About the Cost of Testosterone Replacement Therapy?
By Dr. Kyle Kingsley, MD | Lite Medical PLLC
The cost of testosterone replacement therapy is one of the most frequently searched questions among men considering treatment. At Lite Medical in Minneapolis, testosterone replacement therapy is delivered through a cash-pay model, which means pricing is transparent, known upfront, and not subject to insurance approval, coverage denials, or hidden fees. This guide explains how cash-pay TRT pricing works, what is included in the cost, and how this model compares to insurance-based care.
Understanding the true cost of testosterone replacement therapy requires looking beyond medication price alone. Responsible TRT involves a comprehensive evaluation, ongoing lab monitoring, physician oversight, dosing adjustments, and follow-up consultations. At Lite Medical, every element of care is led by Dr. Kyle Kingsley, MD, and patients know exactly what they are paying for before they begin.
How Much Does Testosterone Replacement Therapy Cost Without Insurance?
The cost of testosterone replacement therapy without insurance varies widely depending on the provider, delivery method, scope of evaluation, and frequency of monitoring. Nationally, men may pay anywhere from a few hundred to several thousand dollars per year for TRT depending on the clinic model and what is included. At Lite Medical, pricing is structured to be transparent, with no hidden costs, no surprise lab fees, and no insurance middlemen influencing clinical decisions.
It is important for men researching the cost of testosterone replacement therapy to understand what a quoted price actually covers. Some clinics advertise low monthly costs that include only the medication itself, while excluding the cost of lab work, physician consultations, follow-up visits, and dosing adjustments. Others bundle everything into a single, predictable fee. The total cost of responsible TRT should reflect the full continuum of care, not just the pharmacy cost of testosterone.
What Is Included in the Cost of TRT at a Cash-Pay Clinic?
At a physician-led cash-pay clinic like Lite Medical, the cost of testosterone replacement therapy typically includes a comprehensive initial evaluation, baseline and ongoing laboratory testing, physician consultations, individualized treatment planning, medication management, dosing adjustments, and regular follow-up visits. Every component is delivered directly by the physician, not delegated to mid-level providers or automated systems.
The initial evaluation at Lite Medical begins with the Premier Discovery Intake, which captures a detailed health history, symptom assessment, current medications, lifestyle factors, and prior lab work. Laboratory assessment includes total testosterone, free testosterone, sex hormone-binding globulin, luteinizing hormone, follicle-stimulating hormone, estradiol, complete blood count, metabolic panel, and additional markers as clinically indicated. This comprehensive baseline is essential for accurate diagnosis and safe treatment planning.
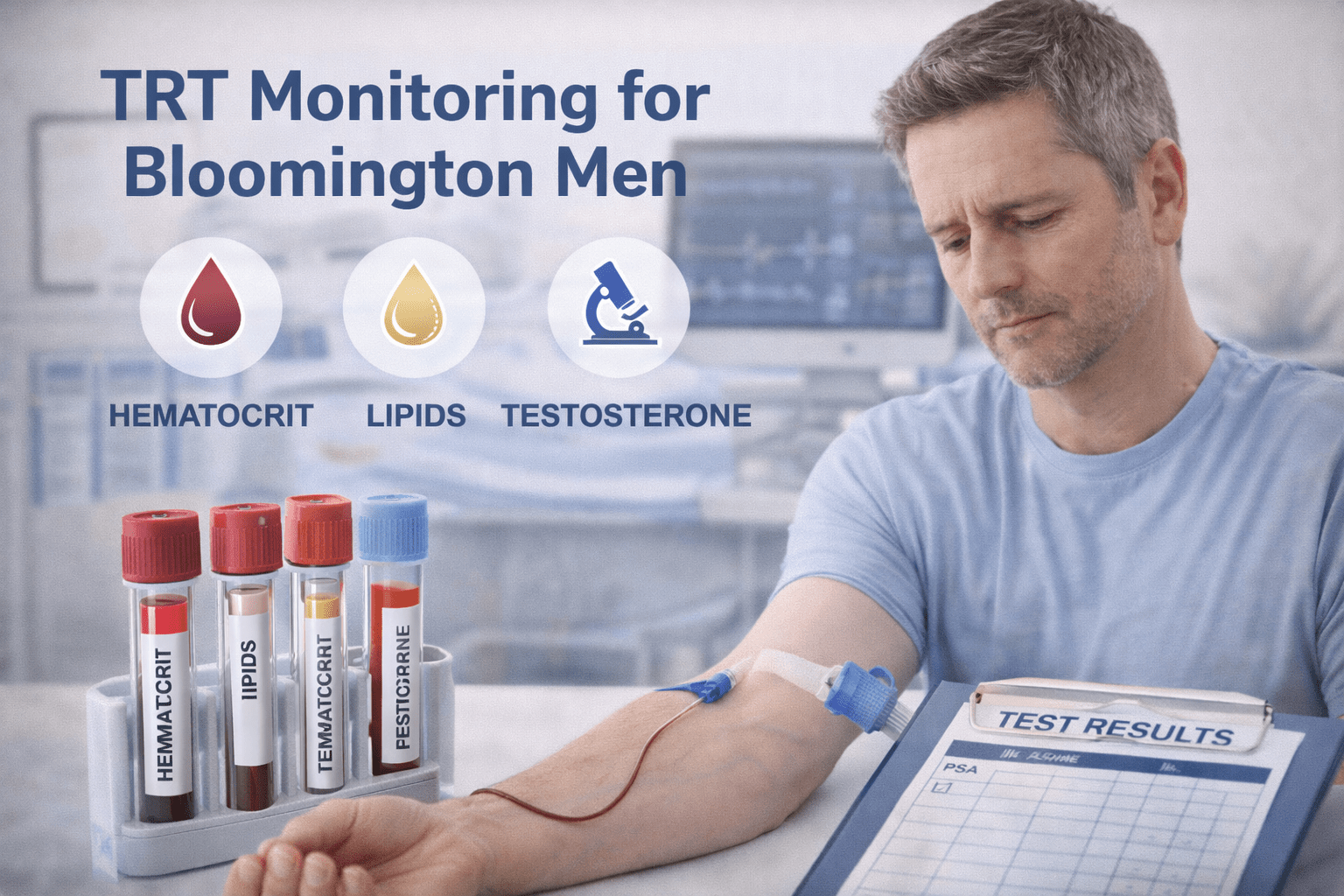
Ongoing care includes periodic lab work to monitor testosterone levels, hematocrit, PSA, lipids, and other relevant markers. Dosing adjustments are made based on both laboratory findings and clinical response. Follow-up consultations with Dr. Kingsley provide the opportunity to review progress, address concerns, and refine the treatment approach over time. This is what responsible testosterone replacement therapy looks like, and it is what the cost should reflect.
How Does Cash-Pay TRT Compare to Insurance-Based Testosterone Therapy?
Cash-pay testosterone replacement therapy differs from insurance-based care in several important ways. In an insurance-based model, coverage for testosterone therapy is subject to prior authorization, formulary restrictions, and step-therapy requirements that may limit which medications or delivery methods are available. Insurance may also restrict the frequency of lab monitoring or the number of follow-up visits covered within a given period.
In a cash-pay model, clinical decisions are made entirely between the physician and the patient. The physician selects the most appropriate delivery method, orders lab work based on clinical judgment rather than coverage rules, and schedules follow-up at intervals that serve the patient’s medical needs. There are no prior authorizations, no coverage denials, and no surprise bills from out-of-network lab facilities.
The International Society for the Study of Women’s Sexual Health (ISSWSH) and other professional organizations have noted that insurance barriers can delay or prevent access to appropriate hormone therapy. While ISSWSH focuses primarily on women’s hormonal health, the principle applies broadly: when insurance dictates treatment parameters, patients may not receive the most clinically appropriate care. This is a central reason why Lite Medical operates on a cash-pay model.
Why Does Transparent Pricing Matter for Testosterone Therapy?
Transparent pricing matters because testosterone replacement therapy is an ongoing medical commitment. Men who begin TRT need to understand the full financial picture before starting, including the cost of evaluation, lab work, medication, and follow-up. Hidden costs or unpredictable billing create barriers to consistent care, which can compromise both safety and outcomes.
At Lite Medical, patients are informed of all costs before any treatment begins. There are no co-pays that change without notice, no balance billing from third-party laboratories, and no administrative fees buried in fine print. This predictability allows men to maintain the continuity that responsible testosterone management requires.
Does the Delivery Method Affect the Cost of TRT?
Yes, the delivery method for testosterone replacement therapy can affect overall cost. Intramuscular injections are generally the most cost-effective delivery method. Transdermal gels and patches, subcutaneous pellets, and nasal formulations each carry different price points based on the medication itself, the frequency of application, and the clinical support required for administration and monitoring.
The choice of delivery method at Lite Medical is a clinical decision made between the physician and the patient based on absorption profile, lifestyle considerations, convenience, and potential side effects. Cost is one factor in the conversation, but it is never the sole driver of clinical decisions. A review in the New England Journal of Medicine (NEJM) has noted the importance of selecting testosterone delivery methods based on individual patient characteristics and clinical goals, reinforcing that the most appropriate method varies by patient.
At Lite Medical, our testosterone replacement therapy program provides clear information about the cost differences between delivery methods so that patients can make informed decisions in partnership with their physician.
What Should I Expect at Lite Medical in Minneapolis?
Lite Medical is a physician-led, cash-pay practice where every patient works directly with Dr. Kyle Kingsley, MD. There are no mid-level providers, no automated treatment pathways, and no insurance-driven restrictions on evaluation scope or physician time. The cash-pay model is designed for men who want straightforward pricing and a care plan built around their individual clinical needs.
Our Minneapolis clinic provides a private, comfortable setting for evaluation and ongoing testosterone therapy. For men in the south metro area, our Edina location offers a physician-led standard of care with a transparent pricing structure.
If you are considering testosterone replacement therapy and want to understand the full cost before committing, our Premier Discovery Intake is the first step. You will receive a comprehensive evaluation, clear pricing, and an individualized treatment plan developed by a physician who will manage your care directly.
Is Testosterone Replacement Therapy Worth the Cost?
Whether testosterone replacement therapy is worth the cost depends on the individual’s clinical situation, the severity of symptoms, and the impact of testosterone deficiency on daily function and quality of life. For men with confirmed deficiency and significant symptoms, physician-led TRT addresses a medical condition. The value of treatment should be evaluated in the context of what is included, the quality of physician oversight, and the long-term safety of the approach.
Men should be cautious about evaluating TRT cost based solely on the lowest advertised price. Programs that minimize physician involvement, skip comprehensive lab work, or use unsupervised protocols may appear less expensive but can introduce safety risks. The cost of responsible testosterone replacement therapy reflects the full scope of care required to manage the condition safely.
Important Safety Information
The US FDA urges caution around unapproved or compounded hormone formulations that may be unsafe. This article is for informational purposes only and does not constitute medical advice. Pricing may vary and is subject to change. Individual results vary, and no specific outcomes are guaranteed. All treatment decisions should be made in consultation with a qualified physician.
Frequently Asked Questions
How much does testosterone replacement therapy cost per month?
The monthly cost of testosterone replacement therapy varies depending on the delivery method, the frequency of lab monitoring, and the clinic model. At Lite Medical, pricing is transparent and discussed before treatment begins so there are no surprises.
Does Lite Medical accept insurance for TRT?
Lite Medical is a cash-pay practice. This model provides transparent pricing, direct physician access, and clinical decisions not subject to insurance approval or formulary restrictions.
What is included in the cost of TRT at Lite Medical?
The cost includes a comprehensive initial evaluation, baseline and ongoing lab work, physician consultations, treatment planning, medication management, dosing adjustments, and regular follow-up visits with Dr. Kingsley.
Are there hidden fees for lab work or follow-up visits?
No. At Lite Medical, all costs are disclosed upfront. There are no hidden lab fees, surprise bills, or administrative charges beyond what is communicated before treatment begins.
Is injectable testosterone cheaper than gels or pellets?
Intramuscular testosterone injections are generally the most cost-effective delivery method. Gels, patches, pellets, and nasal formulations carry different price points. Your physician will discuss the clinical and financial considerations of each option.
Can I get a cost estimate before starting treatment?
Yes. Lite Medical provides a clear cost breakdown before any treatment begins. The Premier Discovery Intake is the first step, and pricing is reviewed as part of that process.